Services on Demand
Journal
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Dental Journal
On-line version ISSN 0375-1562Print version ISSN 0011-8516
S. Afr. dent. j. vol.79 n.8 Johannesburg Sep. 2024
EVIDENCE BASED DENTISTRY
What's new for the clinician - summaries of recently published papers (September 2024)
V Yengopal
Faculty of Dentistry, University of the Western Cape
1. GINGIVAL HEALTH AND RELAPSE TENDENCY OF LOWER FIXED RETAINERS: A RANDOMISED CLINICAL TRIAL
The retention phase after orthodontic treatment is important to obtain stable results.1 Some degree of relapse after treatment can occur, since teeth have a tendency to return towards their original positions.1 Studies have shown that that the design of the retainer can influence both gingival health and the tendency for relapse. For instance, multistrand wire retainers are associated with better alignment retention but may also lead to higher plaque accumulation and gingival irritation compared to single-span retainers. Many types of orthodontic retainers are used after orthodontic treatment including removable (acrylic retainers, vacuum-formed retainers) and fixed bonded retainers. The two most used fixed retainers are the thick (0.025 to 0.032 inch) stainless-steel wire bonded solely to the canines and the thin (0.0175 or 0.0215 inch) multistranded wire bonded to the incisors and canines. The latter type is the most preferred fixed retainers as these are bonded to every tooth in the labial segment.1
Although the impact of a fixed retainer on the gingival health has been extensively studied,1 there is very little evidence to determine the effect of the retainers' position on the periodontal health. Moreover, there is no evidence on the effect of retainers' position on their efficiency and failure rate.
Al-Nimri and colleagues (2024)1 reported on a split mouth randomised clinical trial that sought to study the effect of retainers' position on the periodontal health of the lower anterior teeth, the retention efficacy and the failure rate.
Materials and methods
This was a single-centre split mouth randomised clinical trial study. Fifty adult patients who provided informed consent were randomly selected from a pool of patients scheduled for debonding of orthodontic fixed appliances who also required bonded retention for the lower labial segment. Inclusion criteria were: medically fit Caucasian patients; patients whose treatment plan did not involve extraction of lower anterior teeth; those patients who had well-aligned lower incisors with normal overjet and overbite. Patients were excluded if they had missing lower anterior teeth; history of previous orthodontic treatment; evidence of active periodontal disease; transposition between lower lateral incisor and canine; patient received scaling and root cleaning after retainer placement; patients with parafunctional habits such as nail biting or abnormal tongue function.
At the debonding visit, each patient received a thorough scaling by the same clinician. The appliance was then
debonded and a retainer was attached to all the teeth in the lower labial segment using Transbond LR composite. The retainer has a vertical step in the midline placing half of the retainer in the incisal third and the other half in the middle of the lower labial segment teeth (Fig. 1). A standard procedure for fitting each bonded retainer was applied.
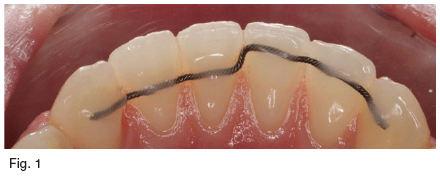
The patients were asked to attend the clinic immediately within 24 hours if the retainer was debonded from any tooth or fractured. Moreover, the patients were recalled on a monthly basis to check for any fractured or debonded retainers not noticed by the patient.
One year after debonding, all subjects were recalled and the Plaque Index (PI) and the Gingival Index (GI) were recorded for the lower anterior teeth. To obtain the PI score, the buccal, lingual, mesial and distal surfaces of the lower anterior teeth were scored from zero to three. The score for each tooth was the sum of the four surfaces divided by four. To calculate PI on the left and right side of the lower labial segment the PI scores for the lower anterior teeth on each side were averaged.
To obtain the GI, the lingual and buccal GI was scored from zero to three. The GI score for each tooth was the sum of buccal and lingual GI divided by two. The GI scores of the lower anterior teeth were summed and averaged to give a GI score for the lower anterior segment on each side of the retainer.
The secondary outcomes were to assess irregularity index (IRI) of the lower anterior teeth and retainers' failure rate. The IRI was determined by using Little's irregularity index to measure the irregularity of the lower anterior teeth.
Results
Fifty-six patients who required bonded retention for the lower anterior segment were assessed for eligibility; 50 of them fulfilled the inclusion criteria and were recruited. Seven patients (14%) were excluded as they failed to attend the clinic at the recall visit. Complete data was collected for 43 patients. In 20 patients the incisal part of the retainer was placed on the right side and in 23 patients the incisal part of the retainer was placed on the left side.
The analysed sample consisted of 29 females and 14 males with an average age of 18.2 years. The trial design was split mouth. This design eliminated the effect of patient oral hygiene on the impact of fixed retainers on gingival health; therefore, the need for baseline data of the oral health was not necessary.
The PI and the GI were smaller on the side where the retainer was placed in the incisal third (1.05 and 0.24, respectively) compared to the side where the retainer was placed in the middle of the tooth (1.30 and 0.40 respectively). This difference was statistically significant (p=0.004 for PI) and (p<0.001 for GI).
The PI was significantly smaller on the lingual (p=0.043), mesial (p=0.020) and distal (p=0.016) surfaces of the lower incisors where the retainer was positioned incisally. Moreover, the GI score was significantly smaller on the lingual surface of the lower incisors on the side where the retainer was placed in the incisal third (p<0.001).
The average IRI on the side with incisally positioned retainer (0.07mm) was not statistically different from that on the side where the retainer was placed in the middle of the lingual surface of the lower labial segment teeth (0.11mm, p=0.194, CI -0.25-0.03). The part of the retainer placed incisal debonded in four subjects (9.3%) while that placed in the middle debonded in Ave subjects (11.6%). The difference was not statistically significant (p=0.52).
Conclusion
The trial results showed that the placing the lower fixed retainers in the incisal third rather than the middle third improved the oral hygiene and the gingival health in the lingual area of the lower labial segment without affecting the efficiency or the integrity of the retainers.
Implications for practice
The trial results showed that simple changes in retainer placement had the potential to improve gingival health and oral hygiene without affecting retainer performance.
REFERENCE
1. Al-Nimri K, Al-Qaqaa S. Gingival health and relapse tendency: a split mouth randomized controlled trial of two positions of lower fixed retainers. Clinical Oral Investigations. 2024 Aug 1;28(8):462 [ Links ]
2. THE DECOMPOSITION AND BLEACHING EFFICIACY OF IN-OFFICE BLEACHING GELS WITH DIFFERENT PH LEVELS: A RANDOMISED CONTROLLED TRIAL
Dental bleaching stands out as one of the most sought-after treatments in cosmetic dentistry. Broadly, there are three main techniques for dental bleaching: in-office, at-home, or a combination of both.1 The in-office method is recommended for individuals who struggle with tray usage or seek more immediate results. While in-office bleaching requires more time at the dentist's office and may lead to more intense side effects compared to at-home methods, it delivers some whitening degree soon after the first session.1
Manufacturers of bleaching products often adopt varying recommendations for applying in-office bleaching gels based on each gel's specific characteristics and the manufacturer's guidelines. Some suggest four cycles lasting 8 min each during a clinical appointment, while others propose three cycles of 15 min each. Additionally, certain bleaching gels are designed for a single application lasting 40 min per clinical session.
The risk and severity of tooth sensitivity (TS) correlate with the duration of the in-office bleaching gel's presence on dental surfaces.1 Gels with an acidic pH can cause various alterations in the chemical composition, structure and mechanical properties of the teeth and, hence, more side effects. Conversely, gels with neutral or alkaline pH levels tend to result in fewer side effects. This emphasises the importance of examining the kinetics of decomposition profile of in-office bleaching gels on contact with dental structures to determine the most effective application time. Doing so we can prevent unnecessary exposure of the gel to the dental tissues, thereby enhancing the procedure's efficacy, speed and safety, and reducing potential side effects.
Gumy and colleagues (2024)1 reported on a trail that sought to assess the decomposition rate and pH alterations of in-office HP gels with varying pH levels during in-office bleaching. The null hypothesis of the present study is that there is no significant difference in (1) the kinetics of decomposition of HP and (2) bleaching efficacy of HP gels between different pHs.
Materials and methods
This was a randomised, double-blind, parallel clinical trial that adhered to the guidelines outlined by the Consolidated Standards of Reporting Trials (CONSORT). The decomposition rate and bleaching efficacy were the dependent variables while the pH of the bleaching gels (pH 5.4, 7.0, 7.7 and 8.0) were the independent variables.
To be eligible for participation in the study, individuals needed to meet specific criteria: they were required to be in good general and oral health, be at least 18 years old, and have incisors, canines and premolars free of caries lesions, restorations or endodontic treatment. Additionally, the baseline Whiteness Index for Dentistry (WID) of the right superior canine, assessed using a digital spectrophotometer (Vita Easyshade), had to be lower than 20, which represented tooth shade A2 in the Vita Classical shade guide. Exclusion criteria encompassed individuals who had previously undergone bleaching procedures, had dental prostheses or exhibited visible enamel cracks. Moreover, individuals with a history of spontaneous tooth hypersensitivity, severe tooth discoloration like tetracycline staining or fluorosis, and those with a history of bruxism were ineligible. Pregnant or lactating women, as well as patients undergoing orthodontic treatment with fixed appliances, were also excluded from participation in the study.
Before the study, predetermined group allocations were logged onto cards, which were then sealed in opaque envelopes numbered from 1 to 40. Each envelope held information regarding the brand of the respective gel. When a participant met the eligibility criteria and initial evaluations were completed, the envelope was opened, revealing the allocation assignment. This method ensured the allocation concealment during the implementation phase. The examiners were not involved in the bleaching procedures and were consequently blinded to the group assignments. Moreover, in this double-blind randomised clinical trial, subjects were also kept unaware of their group assignments.
Forty volunteers were randomly assigned across four groups (n=10): gel with pH 5.4 (Potenza Bianco Pro SS 38%), pH 7.0 (Whiteness HP Automixx 35%); pH 7.7 (Whiteness HP Automixx Plus 35%) and pH 8.0 (Whiteness HP Blue).
The bleaching treatment was administered to all patients by three operators who had undergone calibration. All operators had to perform the bleaching protocol in five patients before the beginning of the study for calibration of all clinical steps. Before the bleaching procedures, all volunteers received dental prophylaxis involving pumice and water applied with a rubber cup, two weeks in advance. Following this, a lip retractor was inserted, and a light-cured resin dam was used to isolate the gingival tissue around the teeth to be bleached. The gingival barrier was individually applied to each tooth and light cured for 20 sec. Subsequently, the assigned bleaching gel was applied in a single 50-min session. This application time was standardised for all materials and determined through randomisation. After completion, the bleaching gel was suctioned using a disposable device, and the teeth were cleaned meticulously with gauze and rinsed thoroughly with water. Two bleaching sessions were conducted, at one-week intervals. Participants were told not to use whitening toothpaste during the study. Instead, they were instructed to use regular toothpaste with fluoride.
For the outcome: Concentration of HP of bleaching agents, the concentration of active HP was evaluated by titration with potassium permanganate at different time intervals: 0, 10, 20, 30, 40, and 50 min at the first session. The bleaching agent was applied first to the premolars and then to the remaining teeth sequentially. Before use, the molar concentration of the potassium permanganate was determined with sodium oxalate. For this study, the concentration obtained was 0.02mol/L.
At each evaluation, an aliquot weighing approximately 0.01g was collected from the premolars with a spatula and weighed on an analytical balance. This amount is equivalent to the gel amount used on each premolar surface. After the removal of the gel, a new layer of HP was placed on the surfaces to not jeopardise bleaching efficacy. Each premolar served as an individual sample, and the gel replaced on its surface was not included in subsequent collections for analysis, meaning that for each time assessment, the collection was done in a different premolar.
The gel was diluted in 20ml of ultrapure water. The diluted bleaching gel was added to 20ml concentrated sulfuric acid 1.0mol/L. The concentration of HP in this solution was determined by titration with 0.02mol/L potassium permanganate. This method was based on an oxidation-reduction reaction and quantifies the amount of HP in the solution. Potassium permanganate was added to the dilute bleaching agent at a rate of 0.1ml/s until a violet colour was observed. The colour change corresponds to the equivalence point when all the HP is consumed.
After each collection, the gel was replaced on the buccal surface of the premolars to avoid colour differences among teeth. The data was presented graphically to observe the changes over time.
For evaluation of the pH change of the bleaching gel, the pH was measured using a pH meter equipped with a circular electrode of 6mm diameter at the same intervals reported in the concentration of HP assessments. Three measurements were taken for each tooth and, subsequently, an average was computed;
For the colour evaluation, two calibrated and trained examiners conducted colour evaluations at specific intervals: baseline, one week after the first bleaching session, one week following the second session, and one month after the bleaching treatment's conclusion. The visual colour assessment employed both the value-oriented shade guide Vita Classical and the Vita Bleached guide 3D-MASTER. Additionally, instrumental colour evaluation was performed using the spectrophotometer Vita Easyshade.
Before spectrophotometer measurement, an impression of the maxillary arch was obtained using condensation silicone (Coltoflax Perfil Cub, Vigodent, Rio de Janeiro, RJ, Brazil) extending to the maxillary canine. To standardise local colour measurement, a 6mm radius window was specifically defined on the labial surface of the silicone guide within the canine area. The three-color parameters: L* (value, 0 [black] to 100 [white]), a* (red-green axis) and b* (yellow-blue axis), were measured using a spectrophotometer.
Colour change was assessed using the Whiteness Index for Dentistry (WID). Higher positive WID values indicated greater tooth whiteness, while lower (even negative) values suggest darker teeth. In addition, AEab (CIELab) and ΔΕ00 (CIEDE2000) were calculated.
Results
Seventy-two participants were examined and 40 were deemed eligible for the clinical study. Gender distribution among the groups was similar as well as baseline colour. The age of patients ranged from 18 to 48 years, with the majority identifying themselves as white.
All participants from the study attended the one-month recall, except one from group pH 7.0 who discontinued treatment before the second session due to intense TS. The data collected from the first session was carried forward for statistical analysis in the intention-to-treat protocol.
Minimal variations, lower than 1%, were observed for the commercial bleaching gels. The pH values of the gels remained consistent with the manufacturers' indications (Whiteness HP Automixx) 7.0 ± 0.2, (Whiteness HP Automixx Plus) 7.7 ± 0.1, and (Whiteness HP Blue) 8.0 ± 0.2, except for the (Potenza Bianco Pro SS) 5.4 ± 0.4, which exhibited values lower than those specified by the manufacturer.
All gels displayed a consistent decline in HP concentration over time, regardless of the pH of the in-office gel. Overall, the decomposition rates were approximately 0.20%, 0.14%, 0.10% and 0.13% per minute for the groups pH 5.4, pH 7.0, pH 7.7 and pH 8.0, respectively.
Throughout the 50-min bleaching period, the gel with pH 8.0 and pH 7.7 groups consistently upheld their pH in the basic range, similarly to the gel with pH 5.4, which retained its acidic nature. Conversely, the gel with pH 7.0 exhibited a distinct behaviour, transitioning from a neutral to an acidic pH.
Neither the interaction of the factors bleaching gel vs time nor the main factor bleaching gel was statistically significant (p>0.05) in all colour evaluation methods. Only the main factor time assessment was statistically significant (p<0.05). The whitening degree of the second session was higher than the first session and equal to the one-month post-bleaching (p<0.05). One month after treatment, all bleaching gels demonstrated a significant increase in the whitening degree in all colour assessment methods.
Conclusion
All bleaching gels kept at least 70% of their HP content after 50 min, suggesting that there is a surplus of HP. They provided similar whitening efficacy one month after bleaching.
Implications for practice
The results of this trial showed it is possible that lower HP concentrations may be equally effective in achieving desired results while reducing the potential for side effects.
REFERENCE
1. Gumy FN, da Silva KL, Gumy MN, Forville H, Cordeiro DC, Favoreto MW, Loguercio AD, Reis A. The decomposition rate and bleaching efficacy of in-office bleaching gels with different pHs: a randomized controlled trial. Clinical Oral Investigations. 2024 Aug;28(8):1-3 explanations. Med Princ Pract 2014; 23: 295-301. [ Links ]













