Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.108 no.6 Pretoria Jun. 2018
http://dx.doi.org/10.7196/samj.2018.v108i6.13373
CME
Managing spinal hypotension during caesarean section: An update
M W GibbsI; D van DykII; R A DyerIII
IMB ChB, DA (SA), FCA (SA), MMed (Anaes); Department of Anaesthesia and Perioperative Medicine, Faculty of Health Sciences, Groote Schuur Hospital and University of Cape Town, South Africa
IIMB ChB, DA (SA), FCA (SA); Department of Anaesthesia and Perioperative Medicine, Faculty of Health Sciences, Groote Schuur Hospital and University of Cape Town, South Africa
IIIFCA (SA), PhD; Department of Anaesthesia and Perioperative Medicine, Faculty of Health Sciences, Groote Schuur Hospital and University of Cape Town, South Africa
ABSTRACT
Hypotension is common after spinal local anaesthesia for caesarean section. However, the substandard treatment of spinal hypotension and associated complications are responsible for up to two-thirds of deaths that occur in South Africa (SA) for caesarean section under spinal anaesthesia. In some cases, spinal hypotension may be predicted by simple parameters such as age >25 years, preoperative heart rate >90 bpm and preoperative mean arterial pressure <90 mmHg. Heart rate variability and point-of-care echocardiography also predict hypotension with greater accuracy, but are limited by equipment and training issues. Spinal anaesthesia is absolutely contraindicated if the parturient is hypovolaemic. Left lateral tilt is still advised, despite the absence of strong supporting evidence. The dose of spinal bupivacaine should not be reduced in obese patients. Crystalloid co-loading is an adequate fluid strategy in most cases, but is of limited efficacy in the prevention of hypotension. It is imperative that immediately after the patient is placed supine, close attention is paid to communication with her, heart rate changes and pulse volume. Early intervention with phenylephrine is the first-line approach for hypotension if heart rate is preserved under spinal anaesthesia. Phenylephrine infusions (25 - 50 μg/min) are easy to administer, maintain baseline maternal haemodynamics and are applicable to the SA context. The vigilant use of phenylephrine boluses (50 - 100 μg), targeting maternal heart rate as a surrogate for cardiac output, is also effective. Noradrenaline has been used successfully to prevent spinal hypotension, but evidence does not yet suggest practice change. Local and international guidelines have recently been published.
What is the magnitude of the problem?
Despite the significant shift in practice from general to spinal anaesthesia for caesarean section, avoidable anaesthetic deaths in South Africa (SA) persist. In the triennium 2011 - 2013, 71% of 105 anaesthesia-related deaths involved spinal anaesthesia, the majority of which were deemed avoidable.[1] Given that more than half (55.1%) of these deaths occurred at district-level hospitals, these institutions should be targeted for support and education, with context-sensitive solutions based on up-to-date evidence-based guidelines.
This brief review summarises the most recent data regarding hypotension during spinal anaesthesia for caesarean section. The authors discuss new insights into the predictors of hypotension, venous and arterial components of haemodynamic changes, dosing controversies and up-to-date treatment modalities.
How do we predict spinal hypotension?
Hypotension after spinal anaesthesia for caesarean section is a common clinical finding and causes major morbidity, and indeed, mortality, depending on the context. Predicting which parturients will experience major spinal hypotension remains a target of ongoing research. In 2014, an in-depth review was published locally, and further recent articles from SA have shed light on the matter. Research has shown a specific pattern of heart rate variability to be a risk factor for spinal hypotension. Bishop et alfi1performed Holter continuous electrocardiogram (ECG) recordings for >5 minutes preoperatively on 102 elective patients due to undergo caesarean section. They investigated the low-frequency/ high-frequency (LFHF) ratio, a measure of heart rate variability, and compared this with baseline heart rate and body mass index (BMI) as other predictors. A logistic regression analysis was performed, which showed that an LFHF threshold of 2.0 was predictive of spinal hypotension (defined as systolic blood pressure <90 mmHg), with an odds ratio of 1.478 (p=0.046). In comparison, BMI and baseline heart rate were less predictive.
A further observational trial by the same authors[3] found that preoperative heart rate, mean arterial pressure (MAP) and maternal age were also predictive of spinal hypotension. A scoring system based on these variables (pulse rate >90 bpm, age >25 years, MAP <90 mmHg - the PRAM score) showed good discrimination, and patients had a 53% chance of developing spinal hypotension if all three factors were present. This simple scoring system, although not validated in larger studies, is probably a more useful practical tool in resource-constrained environments compared with LFHF measurements. In other studies, a BMI >25 kg/m2 has been shown to be a predictor of hypotension, but this was not supported by the PRAM study group.
Recent data showed the benefit of point-of-care echocardiography in the prediction of spinal hypotension. A prospective observational trial assessing changes in the sub-aortic velocity time integral (VTI) after a 45° passive leg raise, found that when the change in VTI was >21%, the area under the receiver operating characteristics (ROC) curve for predicting spinal hypotension was highly predictive at 0.8 (confidence interval 0.6 - 0.9; p=0.0001). Until point-of-care echocardiography and the associated skills become more widely available, this will remain a research tool.
What is the correct spinal anaesthesia dose?
What, then, is the safe and effective dose of intrathecal local anaesthetic? Although a smaller dose is attractive in terms of a lower incidence of hypotension and nausea and vomiting, it is associated with increased breakthrough pain. A meta-analysis of 12 randomised control trials comparing low-dose bupivacaine (i.e. <8 mg/<1.8 mL) with a normal dose of >8 mg, showed a 3-fold increase in the need for analgesic supplementation intraoperatively; the number-needed-to-treat for additional harmful outcomes was 4.[4] Historically, there has been a perception that a non-adjusted spinal dose in obese patients would cause a higher and unpredictable block owing to previous articles suggesting increased block height in such patients. This is concerning in our country, where nearly 70% of women are overweight or obese. After a recent article suggesting that the effective dose 95% (ED95) for intrathecal local anaesthesia for obese and normal BMI parturients is similar, a 2016 study performed by Ngaka et al.[51 specifically addressed this issue. These authors compared a group of patients at term with a BMI of <32 kg/m2 with another whose BMI was >40 kg/m2, each receiving identical doses of local anaesthetic. Although the temperature block was two dermatomes higher at 25 minutes in the morbidly obese group, and there was a 20-minute greater block regression time, there were no block levels higher than T1, and no differences in phenylephrine requirements or in reduction of peak flow rate after spinal anaesthesia. Other studies showed no correlation between height, weight, BMI and block height with standard (12 mg) doses of spinal bupivacaine. Subsequent reviews have thus concluded that dose adjustment of hyperbaric bupivacaine is unnecessary in obese patients.
What is the effect of aortocaval compression on spinal hypotension?
Left lateral tilt (15°) of the parturient after spinal anaesthesia to ensure displacement of the gravid uterus and subsequent aortocaval compression has been standard practice since the 1970s. Lee et al.[6-recently called this practice into question, randomising 100 women to either the supine position or 15° left lateral tilt. Maternal blood pressure was maintained with titrated phenylephrine infusions or boluses in both groups. There was no difference in the primary outcome, i.e. neonatal acid base balance. However, the mean phenyl-ephrine requirement was higher and mean cardiac output decreased in the supine group. An accompanying editorial urges caution in abandoning the classic approach, as some patients have an exaggerated response to aortocaval compression, including occasional reflex bradycardia and precipitous hypotension.
How does the venous circulation affect spinal hypotension?
Due to the physiological changes of pregnancy, healthy women at term have an increase in plasma volume of ~40%, which usually compensates for the sympathectomy associated with spinal anaesthesia. However, after haemorrhage, sympathectomy, as well as the usual arteriolar dilatation associated with spinal anaesthesia, results in venodilatation and rapid decompensation as blood shifts from the stressed volume to the unstressed volume in the splanchnic circulation.
In a recent meta-analysis, Melchor et al.[7] demonstrated that the use of colloids, either as a preload or a co-load, is associated with significantly reduced rates of hypotension compared with crystalloids. However, no method of fluid administration effectively prevents hypotension. Therefore, additional means of maintaining maternal blood pressure are required. In the past 10 - 12 years, research focused on the arterial component of spinal hypotension, the effect of regional anaesthesia on the systemic vascular resistance (SVR) in both healthy women and those with pre-eclampsia, as well as the physiological effect of vasopressors on the SVR. In healthy
women undergoing caesarean section under spinal anaesthesia, minimally invasive cardiac output measurements showed that when the MAP decreases by 20%, the SVR decreases by 35% and the heart rate, stroke volume and cardiac output increase by 12%, 9% and 22%, respectively.[8] The same article showed that phenylephrine restores haemodynamics to baseline, compared with ephedrine, which further increases cardiac output and is associated with a delay to peak pressor effect (undesirable in terms of nausea and vomiting).
There is little information on the effects of spinal anaesthesia on the venous circulation in the fluid-replete parturient. Kuhn et al.[9] used leg wrapping after spinal anaesthesia to reduce hypotension instead of no intervention, and showed that venodilatation does contribute to spinal hypotension. This was, however, a far lesser effect than that of the arteriolar component, and of the effect of phenylephrine infusion in counteracting this decrease in SVR.
Why should phenylephrine be used in spinal hypotension?
It is now well accepted that the best approach to spinal hypotension is by means of a combination of intravenous crystalloid co-load and phenylephrine. This is the most effective method of ensuring maternal safety and comfort and preventing neonatal acidosis. In a randomised double-blind trial comparing varying set rates of phenylephrine infusion, 100 μg/min decreased maternal cardiac output and heart rate by up to 20%. An infusion at a rate of 25 - 50 μg/min was therefore sufficient to maintain appropriate maternal haemodynamics without exposing the fetus to large doses of phenylephrine and is the current recommendation. Although ephedrine is a commonly used drug in the management of spinal hypotension, it has concerning effects on the fetus as a result of stimulation of fetal metabolism after placental transfer of ephedrine and the resulting stimulation of fetal beta-adrenergic receptors. In a study of 109 elective caesarean section patients at term comparing high-dose ephedrine with phenylephrine infusions, titrating the latter to systolic blood pressure resulted in better fetal blood gases (umbilical artery pH 7.25 v. 7.34, base deficit -4.8 v. -1.9 mmol/L, and lactate 4.2 v. 2.2 mmol/L, respectively). A recent meta-analysis reported a 5-fold increase in the risk of fetal acidosis and larger base deficit with ephedrine than with phenylephrine.[10]
A recent randomised trial on the haemodynamics of vasopressors during spinal anaesthesia in cases of pre-eclampsia, demonstrated a significant difference in the effect of vasopressors on SVR, with phenylephrine rapidly restoring SVR to baseline, and ephedrine, even in large doses, being less effective. Phenylephrine also reduces cardiac output, but as an appropriate response to the increase in cardiac output resulting from the spinal anaesthesia (Fig. 1).[11]
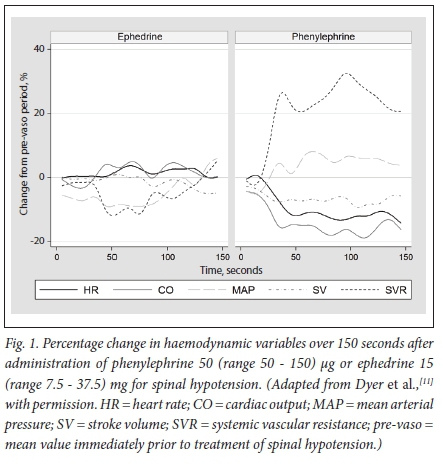
Another trial comparing two groups of women with severe pre-eclampsia and fetal compromise, who were treated with ephedrine and phenylephrine boluses, revealed no significant differences in the primary outcome of umbilical artery base excess (mean -4.9 (standard deviation (SD) 3.7) v. -6.0 (4.6) mmol/L for ephedrine and phenylephrine, respectively; p=0.29).[12] There were also no differences in 1-minute Apgar scores or lactate levels, suggesting that in women with severe pre-eclampsia and fetal compromise, the choice of vasopressor does not affect fetal acid base status.
Anaesthetists should also bear in mind that cardiac output response to phenylephrine is preload dependent. Work done in a porcine general anaesthesia model demonstrated that cardiac output decreases in response to phenylephrine administration when the patient is fluid replete and increases if the animal is fluid depleted.
Therefore, what is the best method of administering phenyl-ephrine? Simple titrated phenylephrine infusions initiated immedi-
ately after the induction of spinal anaesthesia are certainly less labour intensive, are safe and are associated with a low incidence of maternal nausea and vomiting. Closed-loop, feedback computer-controlled phenylephrine infusions provide even tighter blood pressure control. However, this method requires specialised equipment and is not practicable in limited-resource environments. Phenylephrine boluses (50 - 100 μg) may be equally effective in preventing and treating spinal hypotension. The importance lies in choosing the best method appropriate to the maternal condition, local context and physician skill and experience. All the potential administration methods and doses have been well summarised in a recent review.[13]
Should one consider noradrenaline?
There are now several articles advocating the use of noradrenaline rather than phenylephrine for the treatment of spinal hypotension because of its moderate beta-adrenergic effects on maternal heart rate. In a randomised study of 104 healthy patients undergoing caesarean delivery under spinal anaesthesia, at 5 minutes after local anaesthetic injection a noradrenaline infusion maintained maternal cardiac output and heart rate better than a phenylephrine infusion. Maternal blood pressures and neonatal Apgar scores were similar with regard to the relevant infusions. Further work determined that phenylephrine 100 μg equals noradrenaline 8 A subsequent editorial called into question the need for change to a more potent drug, suggesting that the burden of proof for noradrenaline to replace phenylephrine has not as yet been met, in contrast to the proven benefit of phenylephrine over ephedrine.[14]
What is the approach to a patient who develops bradycardia under spinal anaesthesia?
It is imperative that immediately after a spinal local anaesthetic has been injected, close attention is paid to communication with the patient, heart rate changes and pulse volume. Hypotension and bradycardia should be treated with ephedrine and/or anticholinergic agents after increasing left lateral tilt, if necessary.
Bradycardia is not an uncommon occurrence when a patient with spinal hypotension is treated with the enthusiastic administration of phenylephrine. The use of prophylactic glycopyrrolate in conjunction with a phenylephrine infusion was shown to improve cardiac output and heart rate, but at the cost of increased hypertension and an increased incidence of dry mouth. Baroreceptor-mediated bradycardia in response to an increased blood pressure after the administration of phenylephrine should not be treated with anticholinergics, as this may result in tachycardia and hypertension, particularly in pre-eclampsia.
A recent meta-analysis demonstrated that prophylactic ondan-setron reduced the incidence of spinal hypotension, vasopressor consumption and nausea and vomiting in the obstetric and non-obstetric populations, but the clinical significance is uncertain. The exact mechanism is unclear; however, it is suggested that 5-hydroxy-tryptamine (5-HT3)-receptor antagonism during the sympathectomy induced by spinal blockade may decrease the risk of mechanorecep-tor activation in the left ventricle, which could have resulted in the subsequent activation of the Bezold-Jarisch reflex, with hypotension and bradycardia.
Are there any practice guidelines available?
Internationally, a consensus statement has recently been published, which emphasises the importance of pattern recognition of the haemodynamic changes associated with spinal anaesthesia, and describes in detail the management of spinal hypotension with vasopressors during caesarean section.[10] Recommendations for best practice include the use of alpha1-agonists for the treatment and prevention of hypotension (using boluses or infusions); left lateral uterine displacement and crystalloid co-loading or colloid preloading in addition to vasopressors for maintenance of the systolic blood pressure at <90% of baseline, and targeting maternal heart rate as a surrogate marker for cardiac output, i.e. tight haemodynamic control; and the use of phenylephrine infusions at 25 - 50 ug/min immediately after intrathecal injection. In patients with pre-eclampsia, fewer vasopressors are usually required, probably secondary to the vasoconstrictor state associated with this condition.[15-
Guidelines have recently been published on the diagnosis and management of spinal anaesthesia with high sensorimotor block.[16] The main principles remain: (i) preparation for and anticipation of high spinal anaesthesia, including drawing up appropriate drugs; (ii) early recognition; (iii) respiratory support and prompt administration of ephedrine (due to the likelihood of cardiac deafferentation); (iv) avoidance of cardiorespiratory depressants, such as propofol or thiopentone; (v) administration of adrenaline via a peripheral vein if necessary to maintain cardiac output; and (vi) ongoing monitoring of the patient for haemodynamic instability and recovery from respiratory failure.
'Context is king'[17]
Much of the mechanistic research performed on the haemodynamic effects of spinal anaesthesia, and of vasopressors for spinal hypotension, has been carried out in high-resource environments. These findings have greatly improved knowledge and understanding. However, the application of the findings to a resource-limited situation remains challenging. The use of simple phenylephrine infusions has been successfully demonstrated to good effect in the SA context[18] and should encourage SA researchers who are appropriately applying up-to-date information. Ongoing data collection and context-sensitive research are to be encouraged, and audits such as the Confidential Enquiry into Maternal Deaths in SA and initiatives such as the SA Perioperative Research Outcomes Group (SAPORG) are specifically targeting the improvement of obstetric and perinatal care. Given that the recent continent-wide African Surgical Outcomes Study (ASOS) reported caesarean section as the most commonly performed procedure,[19] and that the mortality associated with spinal anaesthesia remains significant, spinal hypotension should ideally be avoided. When it does occur, it is critical that the associated clinical deterioration is immediately identified and appropriate management rapidly initiated.
Key points
• Substandard treatment of spinal hypotension and associated complications are responsible for a large proportion of deaths in SA for caesarean section under spinal anaesthesia.
• Spinal anaesthesia is absolutely contraindicated if the parturient is hypovolaemic.
• Spinal hypotension may in some cases be predicted by simple parameters, such as age, preoperative heart rate and preoperative mean arterial pressure.
• Left lateral tilt is still advised, despite the absence of strong supporting evidence.
• The dose of spinal bupivacaine should not be reduced in obese patients.
• Crystalloid co-loading is an adequate fluid strategy in most cases, but is of limited efficacy in the prevention of hypotension.
• It is imperative that immediately after the patient is placed supine, close attention is paid to communication with her, heart rate changes and pulse volume.
• Early intervention with phenylephrine is the first-line approach for hypotension if the heart rate is preserved under spinal anaesthesia.
• Phenylephrine boluses (50 - 100 μg) or infusions (25 - 50 μg/min) are easy to administer and maintain baseline maternal haemodynamics, and are applicable to the SA context.
• Noradrenaline has been used successfully to prevent spinal hypotension, but evidence does not yet suggest a change of practice.
Acknowledgements. None.
Author contributions. All authors contributed to the intellectual input, contents and editing process.
Funding. None.
Conflicts of interest. None.
References
1. National Committee for the Confidential Enquiries into Maternal Deaths. Saving Mothers 2011 - 2013: Sixth Report on the Confidential Enquiries into Maternal Deaths in South Africa. Pretoria: National Department of Health, 2014. [ Links ]
2. Bishop DG, Cairns C, Grobbelaar M, Rodseth RN. Heart rate variability as a predictor of hypotension following spinal for elective caesarean section: A prospective observational study. Anaesthesia 2017;72(5):603-608. https://doi.org/10.1111/anae.13813 [ Links ]
3. Bishop DG, Cairns C, Grobbelaar M, Rodseth RN. Obstetric spinal hypotension: Preoperative risk factors and the development of a preliminary risk score - the PRAM score. S Afr Med J 2017;107(12):1127-1131. https://doi.org/10.7196/SAMJ.2017.v107i12.12390 [ Links ]
4. Arzola C, Wieczorek PM. Efficacy of low-dose bupivacaine in spinal anaesthesia for caesarean delivery: Systematic review and meta-analysis. Br J Anaesth 2011;107(3):308-318. https://doi.org/10.1093/bja/aer200 [ Links ]
5. Ngaka TC, Coetzee JF, Dyer RA. The influence of body mass index on sensorimotor block and vasopressor requirement during spinal anesthesia for elective cesarean delivery. Anesth Analg 2016;123(6):1527-1534. https://doi.org/10.1213/ANE.0000000000001568 [ Links ]
6. Lee AJ, Landau R, Mattingly JL, et al Left lateral table tilt for elective cesarean delivery under spinal anesthesia has no effect on neonatal acid-base status. Anesthesiology 2017;127(2):241-249. https://doi.org/10.1097/ALN.0000000000001737 [ Links ]
7. Melchor JR, Espinosa A, Hurtado EM, et al. Colloids versus crystalloids in the prevention of cesarean section. A systematic review and meta-analysis. Minerva Anestesiol 2015;81(9):1019-1030. [ Links ]
8. Dyer RA, Reed AR van Dyk D, et al. Hemodynamic effects of ephedrine, phenylephrine, and the coadministration of phenylephrine with oxytocin during spinal anesthesia for elective cesarean delivery. Anesthesiology 2009;111(4):753-766. https://doi.org/10.1097/ALN.0b013e3181b437e0 [ Links ]
9. Kuhn JC, Hauge TH, Rosseland LA, Dahl V, Langesater E. Hemodynamics of phenylephrine infusion versus lower extremity compression during spinal anesthesia for cesarean delivery: A randomized, double-blind, placebo-controlled study. Anesth Analg 2016;122(4):1120-1129. https://doi.org/10.1213/ANE.0000000000001174 [ Links ]
10. Kinsella SM, Carvalho B, Dyer RA, et al. International consensus statement on the management of hypotension with vasopressors during caesarean section under spinal anaesthesia. Anaesthesia 2018;73(1):71-92. https://doi.org/10.1111/anae.14080 [ Links ]
11. Dyer RA, Daniels A, Vorster A, et al. Maternal cardiac output response to colloid preload and vasopressor therapy during spinal anaesthesia for caesarean section in patients with severe preeclampsia: A randomised, controlled trial. Anaesthesia 2018;73(1):23-31. https://doi.org/10.1111/anae.14040 [ Links ]
12. Dyer RA, Emmanuel A, Adams SC, et al. A randomised comparison of bolus phenylephrine and ephedrine for the management of spinal hypotension in patients with severe preeclampsia and fetal compromise. Int J Obstet Anesth 2018;33:23-31. https://doi.org/10.1016/j.ijoa.2017.08.001 [ Links ]
13. Lee JE, George RB, Habib AS. Spinal-induced hypotension: Incidence, mechanisms, prophylaxis, and management: Summarizing 20 years of research. Best Pract Res Clin Anaesthesiol 2017;31(1):57-68. https://doi.org/10.1016/j.bpa.2017.01.001 [ Links ]
14. Carvalho B, Dyer RA. Norepinephrine for spinal hypotension during cesarean delivery: Another paradigm shift? Anesthesiology 2015;122(4):728-730. https://doi.org/10.1097/ALN.0000000000000602 [ Links ]
15. Dyer RA, Piercy JL, Reed AR, Lombard CJ, Schoeman LK, James MF. Hemodynamic changes associated with spinal anesthesia for cesarean delivery in severe preeclampsia. Anesthesiology 2008;108(5):802-811. https://doi.org/10.1097/01.anes.0000311153.84687.c7 [ Links ]
16. Van Rensburg G, van Dyk D, Bishop D, et al. The management of high spinal anaesthesia in obstetrics: Suggested clinical guideline in the South African context. S Afr J Anaesth Analg 2016;22(1) (Suppl 1):51-53. [ Links ]
17. Bishop DG, Rodseth RN, Dyer RA. Context is king - obstetric anaesthesia management strategies in limited resource settings. Int J Obstet Anesth 2017;31:1-4. https://doi.org/10.1016/j.ijoa.2017.04.010 [ Links ]
18. Bishop DG, Cairns C, Grobbelaar M, Rodseth RN. Prophylactic phenylephrine infusions to reduce severe spinal anesthesia hypotension during cesarean delivery in a resource-constrained environment. Anesth Analg 2017;125(3):904-906. https://doi.org/10.1213/ANE.0000000000001905 [ Links ]
19. Biccard BM, Madiba TE, Kluyts H-L, et al. Perioperative patient outcomes in the African Surgical Outcomes Study: A 7-day prospective observational cohort study. Lancet 2018;391(10130):1589-1598. https://doi.org/10.1016/S0140-6736(18)30001-1 [ Links ]
 Correspondence:
Correspondence:
M W Gibbs
matthew.gibbs@uct.ac.za
Accepted 26 April 2018














